U.S. Preventive Services Task Force Expands Access to HIV PrEP, But Inequities Remain a Challenge
08/30/2023
On August 22, the United States Preventive Services Task Force (USPSTF) published new human immunodeficiency virus (HIV) prevention recommendations in JAMA.
Cases of HIV in the United States declined by nearly 10 percent between 2017 and 2021, per the Centers for Disease Control and Prevention (CDC), partially because of expanded access to antiviral medication called pre-exposure prophylaxis (PrEP) — but gross inequities remain an issue.
“Despite these encouraging data, considerable racial, ethnic, and regional disparities in new HIV diagnoses and PrEP use persist in the U.S. and, paradoxically, are worsening as PrEP options and access increase,” experts wrote in an editorial, also published August 22, in JAMA Internal Medicine, about the updated recommendations.
According to James Stevermer, MD, a professor of family and community medicine at the University of Missouri, in Columbia, and a member of the USPSTF who coauthored the new recommendations, “It’s clear that PrEP is not getting out to everyone who could benefit from it. Especially people in the Black and Hispanic communities; these people are not getting prescribed it as much as white patients.”
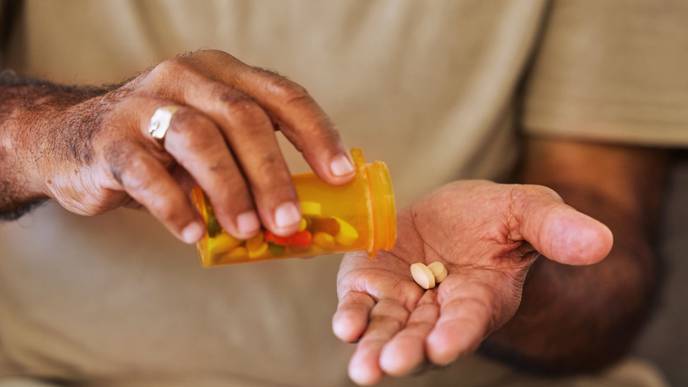
The new recommendations were updated to include all three medications currently approved by the U.S. Food and Drug Administration (FDA) for PrEP — two daily pills, Truvada and Descovy, as well as an injectable called Apretude, which is administered every two months.
“PrEP works a lot better if people take it as they should, so for people who can’t take a daily pill, an injection every couple of months may be a better option to ensure they’re protected against HIV,” says Dr. Stevermer, adding that although these are recommendations, not regulations, they are aimed at helping physicians better treat patients, as well as helping patients access PrEP.
Who Should Take HIV PrEP?
“The USPSTF concludes with high certainty that there is a substantial net benefit from the use of effective antiretroviral therapy to reduce the risk of acquisition of HIV in persons at increased risk of acquiring HIV,” says the recommendation, which applies to adolescents and adults who do not have HIV and are at increased risk of contracting it.
The new guidelines recommend healthcare workers ask patients about their sexual and injection drug use history at every appointment.
According to the task force, doctors should offer PrEP to the following groups:
- Anyone who has a sexual partner with HIV
- Those who’ve had a bacterial sexually transmitted infection within the past six months, such as syphilis, gonorrhea, or chlamydia for men who have sex with men and transgender women, and gonorrhea and syphilis for heterosexual people
- Those who use condoms inconsistently or never
- Anyone who injects drugs or has a sexual partner who injects drugs
People who engage in transactional sex should also be offered PrEP, the guidelines say.
Updated Guidelines Should Expand Access to PrEP
Because all three medications received a “grade A” USPSTF recommendation, the hope is that more people will be able to access the medications, since most private insurance plans are required to cover preventive services that receive a grade of A or B from the USPSTF without a copay. PrEP also must be free under almost all health insurance plans under the Affordable Care Act (ACA).
That expanded coverage is helpful, but not a silver bullet.
“Access to a regular primary care physician is important in getting PrEP, and not everyone has insurance to cover that,” Stevermer says.
Bridging Gaps in PrEP Access
Expanding a person’s choices of medications will likely improve PrEP uptake, but more comprehensive efforts need to be made to make sure these new options are distributed equitably.
The recommendations note that PrEP is underutilized in many communities that could benefit from it, particularly Black and Latino people who are at high risk of contracting HIV.
In 2021, nearly 80 percent of white Americans expected to benefit from PrEP received it. This is a stark contrast to just 11 percent of Black Americans who’d be expected to benefit and 21 percent of Latinos. And while people living in the South accounted for more than half of HIV diagnoses in 2021, they make up less than 40 percent of PrEP users, according to another editorial on the recommendations, also published August 22 in JAMA. PrEP use has also been disproportionately low among cisgender and transgender women, youth, and people who inject drugs.
“The field has changed quickly, and we will have even more medicines in the future. But it will always be a social issue and will need a more anthropologic point of view,” says Kevin Escandón, MD, an HIV doctor and infectious-diseases researcher at the University of Minnesota Medical School in Minneapolis. “We need more work in discrimination and equal rights, because if you don’t have that, even if you have more medications out there, you will have inequities in who has access to those medications.”
The new PrEP recommendations highlighted inadequate research on risk assessment tools that help physicians identify people who are at risk for contracting HIV. According to Dr. Escandón, initiatives such as mobile clinics could help bring PrEP directly to the people who could benefit from it, but first, experts need to better understand the barriers that prevent so many people from accessing HIV prevention.
“We do not think this recommendation alone is going to fix the problem,” Stevermer says. “We’re calling for more research to better reach out to these groups that are not getting adequate access to PrEP.”

Facebook Comments